Pneumonia: The Underrated Risk
A special research team is looking for answers to unsolved questions on pneumococcal disease.
Jun 15, 2017
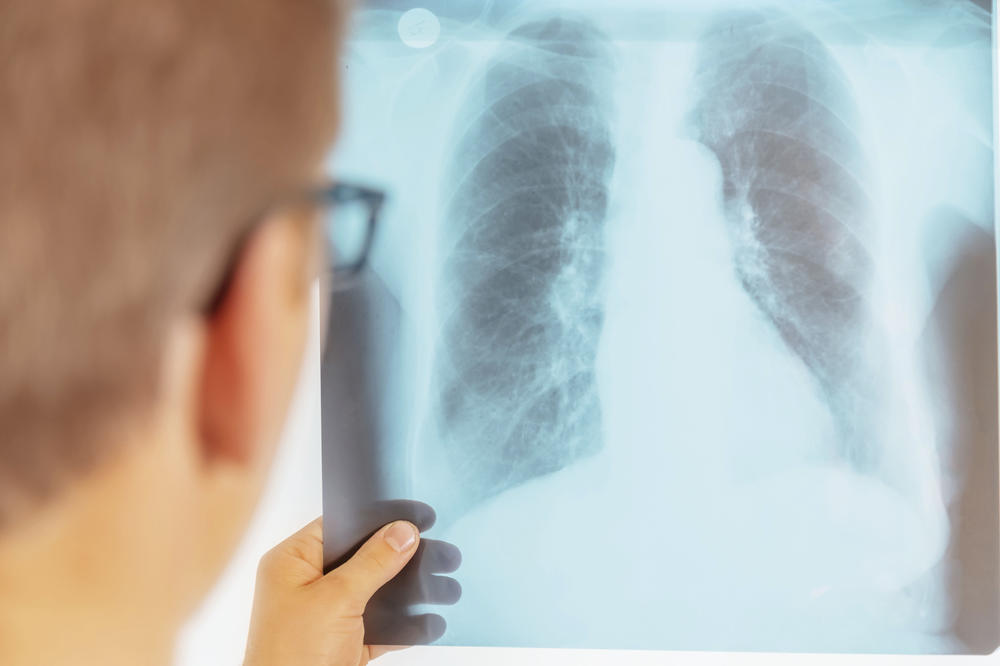
In cases of bacterial pneumonia, inflammation of the lung tissue can often be seen on patients’ X-rays. However, research has yet to be done to see what happens in the lungs when they become infected with pathogens such as pneumococci.
Image Credit: iStockphtoto/Remains
Some 740,000 people in Germany contract pneumonia every year. While most are treated as outpatients, around one third of the cases are so severe that hospital treatment is needed. Despite that treatment and care, 12 percent of patients do not survive. “Pneumonia is becoming as serious as heart attacks and strokes,” says Norbert Suttorp, director of the Medizinische Klinik mit Schwerpunkt Infektiologie und Pneumologie der Charité – Universitätsmedizin Berlin, the university hospital run jointly by Freie Universität and Humboldt-Universität zu Berlin. Why is morbidity so high despite medical progress, and what can be done to stem it?
This is the question that researchers have set out to answer as part of the Transregio 84 Collaborative Research Center (CRC) funded by the German Research Foundation (DFG). The project on congenital immunity of the lung (Angeborene Immunität der Lunge) is now entering its third funding phase. In addition to the Charité university hospital, other project partners include Freie Universität Berlin, the universities of Marburg and Gießen, the Robert Koch Institute, the Max Plank Institute (MPI) for Molecular Genetics in Berlin, and the MPI of Colloids and Interfaces in Potsdam.
Resistance Not Really a Problem in Germany Yet
The research team is looking at how the pathogens attack the body, how the immune system reacts to the infection, and how the disease’s progress can be better assessed. “Here in Germany, resistance to pneumococci – the most important pathogen – is not really a problem like it is in France, Italy, and the U.S.,” says Suttorp, the Transregio 84 spokesperson. This is why the 19 projects involved in the CRC focus not on new antibiotics, but on gaining a detailed insight into what actually happens in the lung when pneumonia occurs.
What the researchers do know is that the lung has to work exceptionally hard to beat the infection. “It has to eliminate a pathogen while ensuring that the gas in the lung’s air sacs is exchanged at intervals of once every second,” Suttorp says. And thanks to high-end microscopy, the research team can watch the alveoli (the air sacs) at work, and not just when fighting pneumococci. They can do this thanks to a key technological program that uses modern imaging and histological techniques.
As the findings of experiments done with laboratory mice cannot be directly transferred to humans, the researchers use human tissue to test whether the results acquired from animal testing have any relevance for human health. They take strips of healthy tissue from the edge of lung flaps removed from tumor patients, infect them with pneumococci, and examine them under laboratory conditions. As the program develops, the researchers aim to use fine jets of water to cut especially thin strips of tissue. Until now, it has been difficult to tell which type of lung cell becomes infected by the influenza virus. “Under the microscope,” Suttorp says, “we can now observe the viruses flitting around the alveolar cells and we can see that only Type II epithelial cells are involved.”
50 Percent Risk of Dying from MERS Corona
The research team is currently investigating a coronavirus from the MERS group. MERS stands for Middle East Respiratory Syndrome, a term used to describe an infection of the respiratory tract which is triggered by a new type of coronavirus. “If we add the virus to our tissue samples, each and every alveolar cell becomes infected,” says Sutton. “That explains why there is a 50 percent of risk of dying from MERS Corona or Mers-CoV.” Experiments like these help to show how the infection’s mechanisms work and thus aid the development of new forms of treatment. The very latest finding shows that, in a similar way to the intestine, the lung is not sterile but populated by microorganisms. Why are those organisms there? How do they interact? Do they perhaps perform a protective function?
These questions are among those being addressed by the Transregio 84 research team. Pneumonia is a special case that often arises following a stroke. “Up to now,” Suttorp says, “it was assumed that it involved aspiration pneumonia, a lung infection caused by a patient’s inability to swallow. But that is not the case. Stroke patients have an immune system paralysis, especially in the lungs.” The immune system more or less goes into shock and a minute fraction of the usual number of germs is enough to cause infection. The immune system has to manage its resources wisely and so deploys its defenses in waves. “If there is only single bacterial molecule in the blood, then it doesn’t have to fight too hard,” Suttorp explains. “But with anything bigger, say a bacterium, then it goes into action and pulls out all the stops.”
Researchers at the Charité university hospital have discovered that the body can actually detect whether an invader is dead or alive. If it is alive, the immune system searches for pathogen-associated molecule patterns within the body, i.e., for other signs of the pathogen’s presence. If the pathogen is found, the immune system sounds the alarm. This is information that can be used in developing new vaccines: live virus vaccines are more effective than killed virus vaccines, but they are less easy to deal with because they require a cool chain that is constant and unbroken.
“We are trying to develop a dead vaccine against pneumococci and to add a pathogen-associated molecule pattern comprising RNA snippets from the bacterium,” Suttorp explains. The latter tricks the immune system into thinking that a live pathogen has entered the body and puts it on the defense. Experts recommend that people aged 60 and over should be vaccinated against pneumococcal disease because the risk of infection increases in old age.
Patients Especially Prone to Severe Pneumococcal Infection
Because the same bacteria are also responsible for meningitis and middle-ear infections, small children are also vaccinated against the disease. And according to Suttorp, their grandparents benefit from this. “A study conducted in the U.S. has shown that pneumonia rates drop among grandparents with grandchildren who have been immunized.” Doctors are desperately searching for parameters that they can use for early detection of patients who are likely to be especially prone to severe pneumococcal infection. Genotyping is thus another important term in Transregio 84 research terminology. How do the genes in patients who suffer severe symptoms, including blood poisoning, and thus need intensive medical care, differ from those in patients with only mild forms of the disease? The search is on for additional biomarkers in the blood which can show the current status of the disease and also predict its future progress.
The role the body’s immune system plays in fighting off a lung infection was shown in the first-ever study on antibiotics involving pneumococcal pneumonia published in The Lancet medical journal back in 1938. In the study, hundreds of patients were treated with a sulfonamide, while those in a control group of the same size were given a placebo. Of those who received placebos, 70 survived. That figure rose to 90 among those treated with an antibiotic. “We’re still working on that final 10 percent,” Suttrop says. “Antibiotics are vital. We’ll always be reliant on them, but we also need additional forms of treatment that help the body to cope even after the bacteria have been killed.”
This article was first published in the Freie Universität Tagesspiegel supplement dated February 13, 2015, and was later revised in June 2017.