Attacking One’s Own Brain
Neurologists at Charité Berlin and their colleagues in Oxford are investigating a new form of brain inflammation — autoimmune encephalitis.
Dec 12, 2018
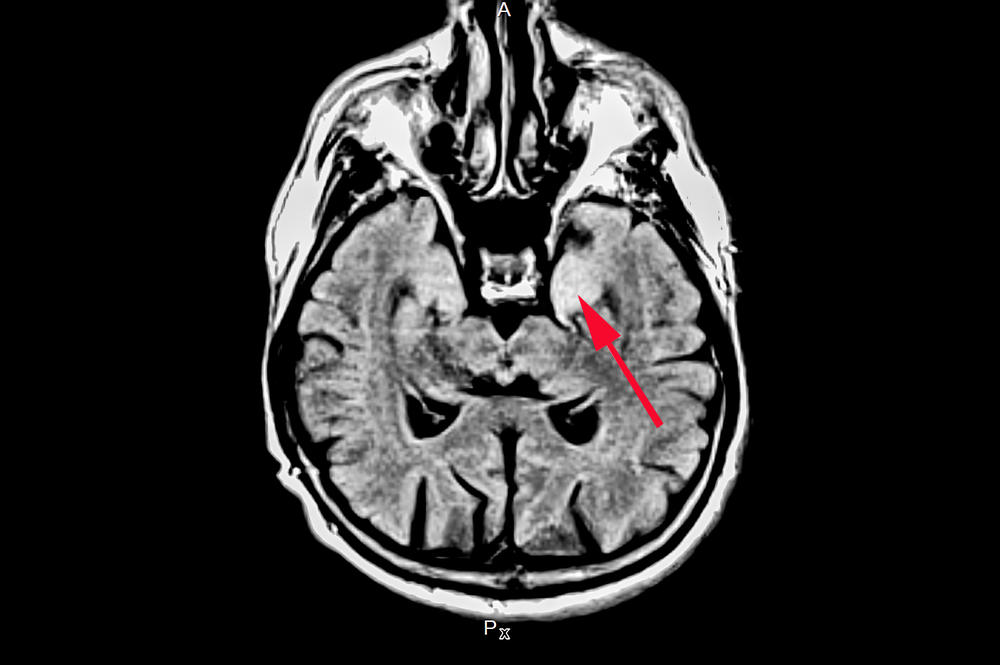
MRI image of a patient with autoimmune brain inflammation: in particular, parts of the temporal lobe (arrow) are especially and frequently affected by the inflammation.
Image Credit: Harald Prüß
It predominantly affects young women and children and often begins with a seemingly harmless infection. The patients feel unwell and have headaches and aching limbs. They then develop a psychosis, which can vary in intensity — with delusions, hallucinations, and even suicidal thoughts. This results in admission to a psychiatric ward, due to the young age of most patients, and a “drug-induced psychosis” is often suspected. “Essentially, those who develop neurological complications are almost lucky: three quarters get epileptic seizures, movement disorders, or impaired consciousness. This is where they turn to neurology, where the right diagnosis is made for the first time,” explains Harald Prüß, a neurologist at Charité – Universitätsmedizin Berlin.
Proving the disease exists is basically simple, Prüß explains: the cerebrospinal fluid contains antibodies against the NMDA receptor, a protein that plays an important role in signal transduction in the brain. “The antibodies lead to the invagination of the receptor into the nerve cell and can thus produce a variegated picture of symptoms in the affected person.” In many cases, it is the image of a severe brain inflammation that requires intensive medical treatment.
Neurologist Harald Prüß is investigating how patients with autoimmune encephalitis can be treated more effectively.
Image Credit: privat
Anti-NMDA receptor autoimmune encephalitis was first diagnosed eleven years ago. This is surprising because it is the most common autoimmune brain inflammation in humans. At Charité, Prüß and his colleagues are investigating what exactly the antibody does. “It appears to work like a drug or a poison, directly harming the nerve cell.” For neurologists, this is a completely new phenomenon that the Berlin research group now wants to investigate further with Sarosh Irani, a medical doctor at Oxford University and his team. Irani also attends patients with autoimmune encephalitis and does research on a similar topic. “We want to find out exactly what the antibodies do,” says Prüß. “What led people to develop them in the first place? And what role do certain immune cells play in this?”
Since the discovery of the first antibody, more than 30 more have been found that cause a similar disease. And every three to six months another one is added. Some bind on to ion channels, others to cell adhesion molecules, proteins that, among other things, enable cells to communicate with each other. Other antibodies even block water channels in the cell wall of neurons. “The operating principles are different, but they all have one thing in common: they start in the brain or the central nervous system and can cause considerable damage there,” explains Harald Prüß.
The sooner the disease is diagnosed and treatment is started, the lower the subsequent damage will be.
How is autoimmune encephalitis treated? First, the antibodies have to come out of the body. This is done through dialysis by means of plasma exchange or immune adsorption, in which plasma is purified of autoantibodies and immune complexes in the bloodstream. However, the danger is not yet averted because the cells producing the antibodies still circulate in the blood. “As a rule, they are removed by prolonged treatment with a monoclonal antibody, known from cancer treatment, that specifically eliminates the targeted cells,” says Prüß. Less than just five percent of patients suffer a relapse afterward.
The success of the treatment in individual cases depends largely on how quickly the disease is diagnosed and the treatment started. If the antibodies are only able to act for a short time, the consequential damage is minimal. “Initially, they only block certain receptors, which the nerve cell can still counterbalance,” explains Prüß. However, if the disease remains untreated for weeks and months, the damage is irreversible.
Even if (fortunately) there are now only a small number of patients with the most severe deficits, most of them have mild impairments, including emotional dysregulation, increased impulsion, or decreased resilience, and they are no longer able to work full time. But many are doing well thanks to the treatment, says Prüß. “So far we have treated over 100 patients with anti-NMDA receptor encephalitis at Charité alone. Three quarters of them were able to return to school or work.”